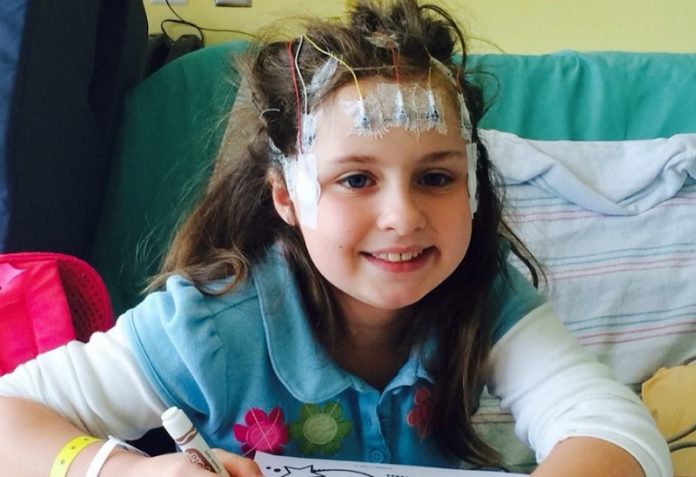
Dhealthwellness.com – Symptoms of Refractory Epilepsy include a loss of control over seizures. These seizures last for several seconds to several minutes. About one-third of epilepsy patients will eventually develop refractory epilepsy, meaning that drugs or therapies do not control the seizures. Your doctor can perform an electroencephalogram to determine whether the seizures are refractory to medicines. If you have refractory partial epilepsy, your doctor can try removing part of the brain that starts seizures.
Correct Diagnosis and Epilepsy Syndrome
Refractory epilepsy patients require extensive assessment and treatment planning, based on a clear diagnosis and appropriate epilepsy syndrome. In addition to AEDs, refractory epilepsy must also be excluded by no other diagnosis, such as the presence of non-epileptic events or poor compliance. This article presents an overview of patient management in daily clinical practice. We hope you find the information presented here helpful.
A patient with refractory epilepsy may have nocturnal seizures or diurnal generalized tonic-clonic seizures. These seizures affect employment, education, and driving. The patient’s refractoriness may evolve from probable to probable refractoriness, depending on the type of AEDs that he or she takes. However, there are predictive factors that should be considered for the diagnosis.
In addition to the Symptoms of Refractory Epilepsy include a loss of control over seizures, genetics may play a role in refractory epilepsy. Genetics are not fully understood, so there is not a clear genetic cause for refractoriness. Genetics, however, are still a strong possibility. However, few studies have examined the genetics of refractory epilepsy. The findings suggest that the genetic makeup of refractory epilepsy can determine whether an individual develops seizures after receiving certain drugs.

The transporter hypothesis focuses on the role of efflux transporters in the drug resistance process. This hypothesis is based on experimental and clinical data that supports overexpression of ABC multidrug efflux transporters. Further studies will be necessary to determine whether the overexpression of P-gp is a contributing factor. For now, this hypothesis is the foundation of pharmacokinetic studies in patients with refractory epilepsy.
Efficacy of Additional P-gp Inhibitors in Refractory Epilepsy
P-gp inhibitors, also known as ligands, may improve seizure control. However, they are relatively unspecific and have not been used in human clinical trials. This means that no definitive conclusions can be drawn about the efficacy of add-on P-gp inhibitors in refractory epilepsy. Further, a large number of patients is needed to obtain statistically significant results.
In addition to genetics, environmental factors, and patient history also influence the outcome of treatment. For example, the underlying syndrome, etiology, and previous history of seizures can all influence the response rate to AED therapy. Environmental factors, including genetics, may also influence the rate of drug uptake in the targeted tissues. When these factors are present, treatment resistance is likely to be highly variable. If the genetics of the patient are not to blame for refractory epilepsy, the use of alternative therapies will be needed.
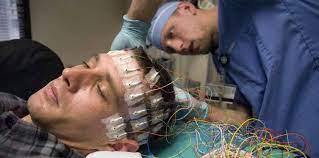
Other potential treatment methods for refractory epilepsy include electrical brain stimulation, polymers, and prediction of seizure occurrence. Cell and gene therapy are still far from routine clinical use. Ultimately, this is a review of the available treatments for refractory epilepsy. We hope this review will help you to make an informed decision when you seek treatment for your condition. Please consider sharing your findings with your health care provider if you’ve had successful outcomes with others!
Newest Treatment for Refractory Epilepsy
Among the newest treatments for refractory epilepsy are pharmacological methods. Molecular genetic tests may help in choosing the right epilepsy medication for you. For instance, some patients have abnormal levels of ABCB1 protein. If this is the case, an ABCB1-related polymorphism might be a surrogate marker for refractory epilepsy. Alternatively, your doctor may want to try a genetic test to determine if P-gp protein is overexpressed.
Another common form of refractory epilepsy involves a death from a non-traumatic cause. The death of an epilepsy patient can be devastating. Statistics show that it can affect a person’s social status, physical health, and psychological outcomes. Approximately one-third of people with this disorder will have a seizure at some point in their life, with most deaths coming from refractory epilepsy.
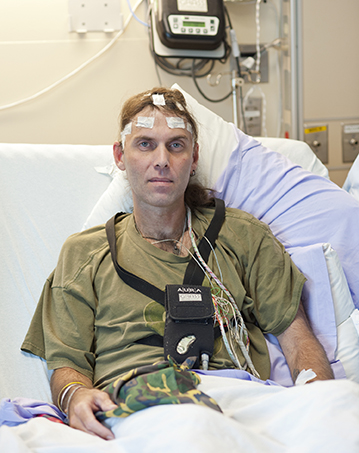 Another treatment for refractory epilepsy involves surgically removing part of the brain. This surgical procedure is known as a lesionectomy. It removes part of the cortex. While the brain does not have the capacity to heal itself, a refractory patient may require several surgeries before the disease stabilizes. A lesionectomy without a cortical margin is a more effective treatment than continuing pharmacotherapy.
Another treatment for refractory epilepsy involves surgically removing part of the brain. This surgical procedure is known as a lesionectomy. It removes part of the cortex. While the brain does not have the capacity to heal itself, a refractory patient may require several surgeries before the disease stabilizes. A lesionectomy without a cortical margin is a more effective treatment than continuing pharmacotherapy.
Reference: