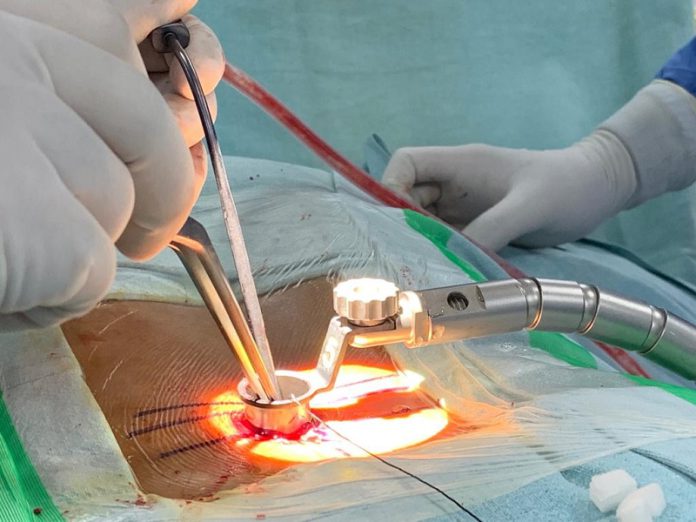
Dhealthwellness.com – A Pedicle Probe provides tactile feedback for surgeons during spinal surgery. Without this feedback, resident surgeons cannot gain a full understanding of the procedure and are limited in their skill. Additionally, the lack of a feedback device increases the risk of catastrophic failure. A Pedicle Probe provides an accurate measurement of forces and allows surgeons to predict if the pedicle is about to breach or not. To understand the potential risk of pedicle breach, a surgeon should first understand the anatomy and physiology of spinal deformity.
Pedicle Probe Anatomy
The anatomy of a Pedicle Probe focuses on the exact sagittal and transverse angles, anatomical structures of each vertebra, and proper entry points for pedicle screws. A Pedicle Probe enables surgeons to ensure a proper placement and ensure the integrity of the pedicle channels. Furthermore, it allows surgeons to check whether pedicle screws are inserted correctly to avoid perforation and damage to the spinal cord.
Typically, 90% of pedicles are large cancellous channels, and they are easily accessible with a Pedicle Probe. The method of inserting a Pedicle Probe uses a flexible drill bit that deflects off the cortical walls and self-centers in the cancellous center. Some authors advocate hammering the probe through the pedicle through the cortical walls, but there are other methods, such as a rigid drill using controlled force and excursion.
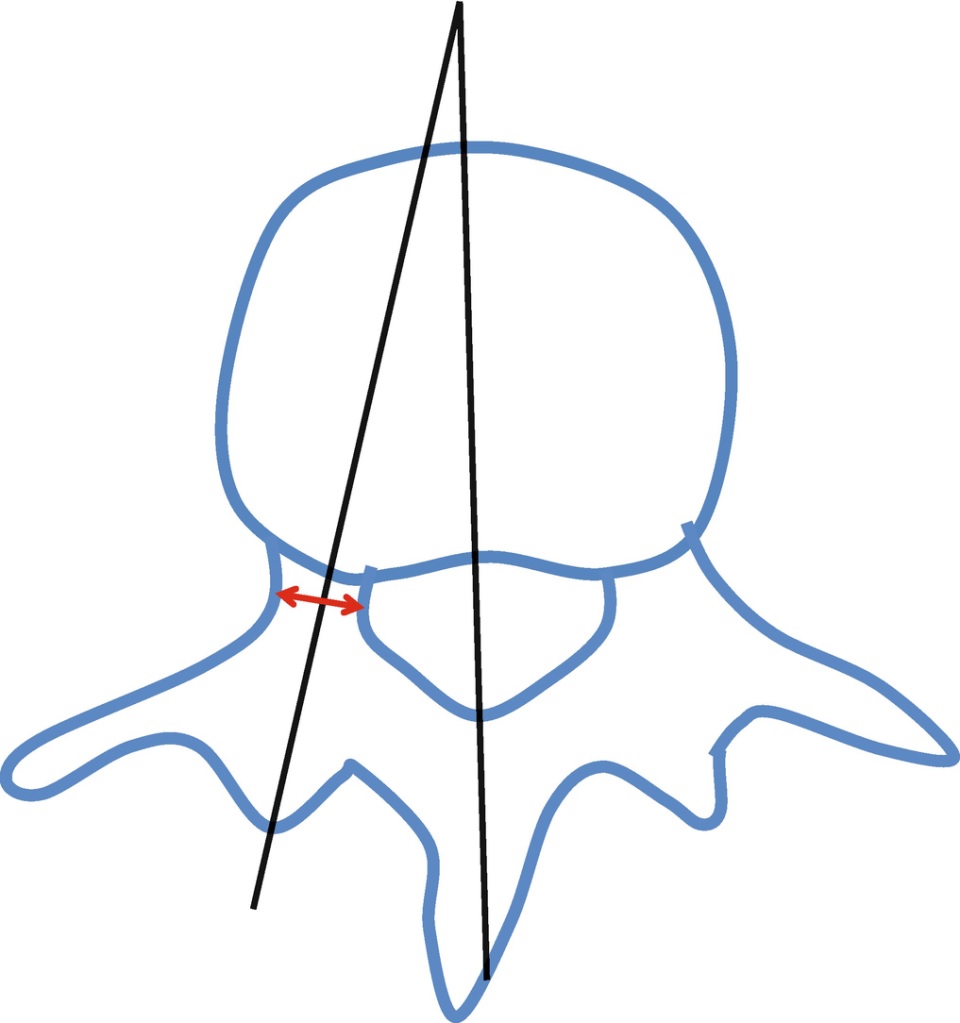
A spinal probe is an instrument that is able to navigate through a pedicle, which is the body of a vertebra. The probe is designed to travel through a cancellous bone, where it would meet resistance. When it encounters resistance, the probe is stopped. It would then rotate 180 degrees and reach the cortex at the medial margin of the pedicle. Once the probe had reached the cortex, it would then be rotated by 180 degrees and reduce in angle, continuing to penetrate the vertebrae body.
Measuring Pedicle Duct Procedures Accurately
A cadaver study demonstrated that a Pedicle Probe has the ability to accurately quantify pedicle tract procedures. The data obtained from the cadaver study showed the range of forces experienced during a typical pedicle tract procedure. A lateral breach of the right pedicle in L5 produced the highest radial force, with a standard deviation of 2.50 lbf. The intact placement of the Pedicle Probe in T12 was the lowest. The probe also had characteristic “target signs” during the pedicle tract procedure.
A second embodiment of the Pedicle Probe captures forces at the tip of the spinal awl. This configuration eliminates the need for a separate force sensor on the awl’s handle. The second embodiment of the Pedicle Probe includes a load cell that can measure six degrees of freedom and moments. The device is similar in size, shape, and weight to existing spinal probes. Because it can capture multiple forces, it is useful in spine surgery.
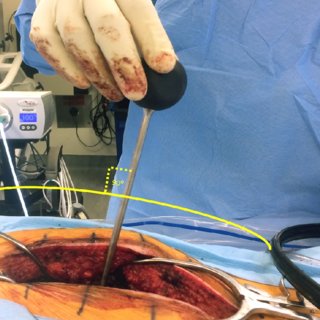
To determine if a Pedicle Probe can successfully penetrate the cortex of the pedicle, the awl tip was tapered to create an effective force sensor. These frictional forces were translated into force values via the load cell on the smart probe. This measurement validated the use of the twisting method and helped determine its mechanical advantage. This study also demonstrated that Pedicle Probes can detect pedicles that are deeper than the awl can reach.
The Best Way to Distinguish between Intact and Broken Pedicles
One study evaluated the accuracy of the Pedicle Probe on eight postmortem pig spines. The researchers determined the best way to differentiate between an intact and breached pedicle. The Pedicle Probe was more accurate than a curved pedicle probe. A successful Pedicle Probe is more reliable than a Pedicle MRI. It is useful for determining the sagittal position of the spine, the pedicle’s transverse diameter, and the screw trajectory.
Once the data collection is complete, the data collection process can be regulated by the software user interface. The data collected is displayed as a graph or as a series of icons. In one display, vertical bars illuminate as the probe approaches the boundary. Afterwards, the data can be saved to a text file. If necessary, the data can be analyzed and compared. The research further shows that the Pedicle Probe has high accuracy.
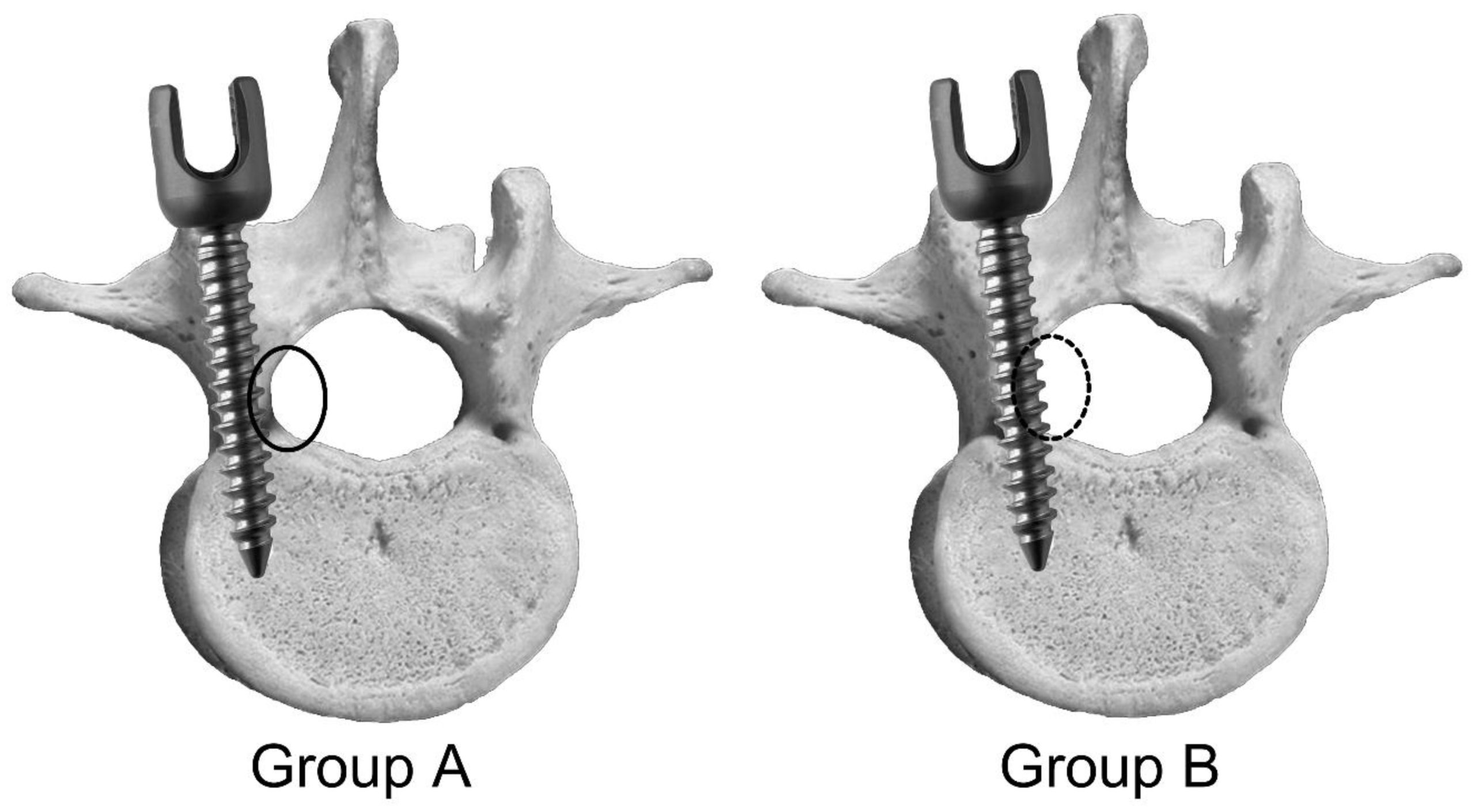
The predictive algorithm was based on the mean radial force of previous successful procedures. Past successful samples were used as the population mean and the standard deviation. These values were used to calculate the 95% confidence interval of pedicle tract procedures. The first predictive algorithm uses the population mean as the radial force of successful samples. The second predictive algorithm uses the average axial force of successful pedicles. The predictive algorithm also considers the number of pedicles and the number of procedures.
Reference: