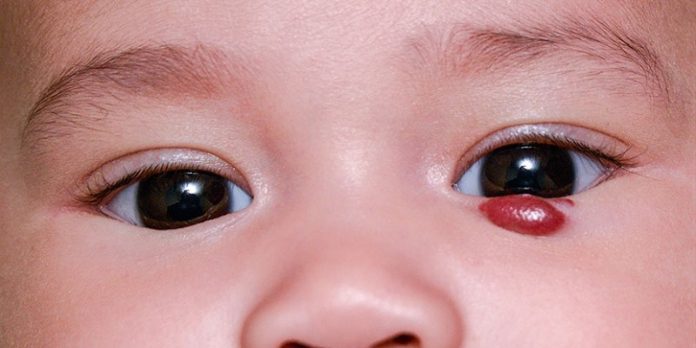
Dhealthwellness.com – Hemangiomas are benign skin growths that start as faint red birthmarks and grow rapidly to a larger size. Unlike vascular malformations, which grow slowly, hemangiomas usually grow rapidly. The healthcare provider will examine your child’s skin to determine the exact cause of your child’s growth. A doctor may use ultrasound to identify hemangiomas. Treatment for hemangiomas depends on the type of growth, the age of your child, and the severity of the lesion.
Recommend Treatment for Hemangiomas
Treatment for hemangiomas can include observation, drug therapy, or surgery. While hemangiomas that occur in infancy usually shrink and are not painful, they may block breathing or vision and can be cosmetically unappealing. A pediatrician may recommend either surgical removal or drug therapy to address your child’s hemangiomas. If hemangiomas become large, however, they may require surgical removal.
A biopsy is another way to confirm a hemangioma diagnosis. A sample of tissue is taken and examined under a microscope to determine its type and subtype. A local anesthetic is used to numb the area being biopsyed. The biopsy is a minor operation and is usually done in a hospital. Blood tests can also help diagnose hemangiomas. If you suspect you have a hemangioma, contact your healthcare provider immediately.
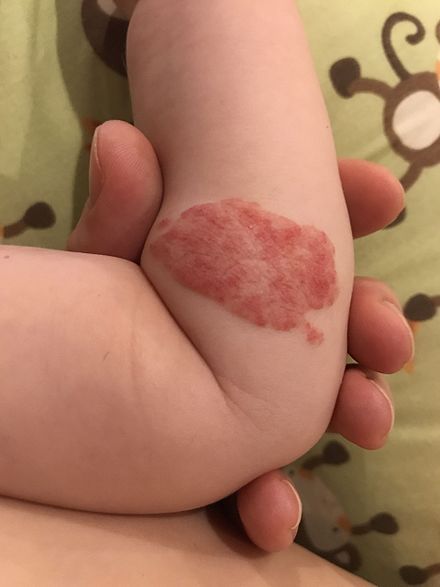
Hemangiomas are the most common type of childhood tumor. They affect about five percent of children and are more likely to occur in white kids. Approximately 80 percent of hemangiomas will reach their full size by three to five months of age, and most will be gone by the time your child turns one year old. Hemangiomas can develop anywhere on your child’s skin, although they are most commonly found in the cheeks and upper eyelids. They will often fade, but they may leave discolored or scarred skin behind.
Benign Tumors Consisting of Blood Vessels
A hemangioma is a benign tumor made up of blood vessels. These tumors can occur on any part of your body, but they are more common in Caucasians and girls. Hemangiomas may be accompanied by a wide range of symptoms and are often treated surgically. However, they can interfere with breathing. Therefore, the best treatment is a complete medical evaluation. So, don’t wait another second – schedule your appointment with a qualified pediatrician today.
Infantile hemangiomas typically grow for six to twelve months. They may initially appear as a red birthmark. But, by the time your child is three to four months old, they will be more prominent and may protrude from the skin. Some hemangiomas are deep and appear under the skin. The size of your child’s hemangiomas depends on its location. Although rarely hereditary, you can be sure that your child will grow up with this condition if you are diagnosed with it.
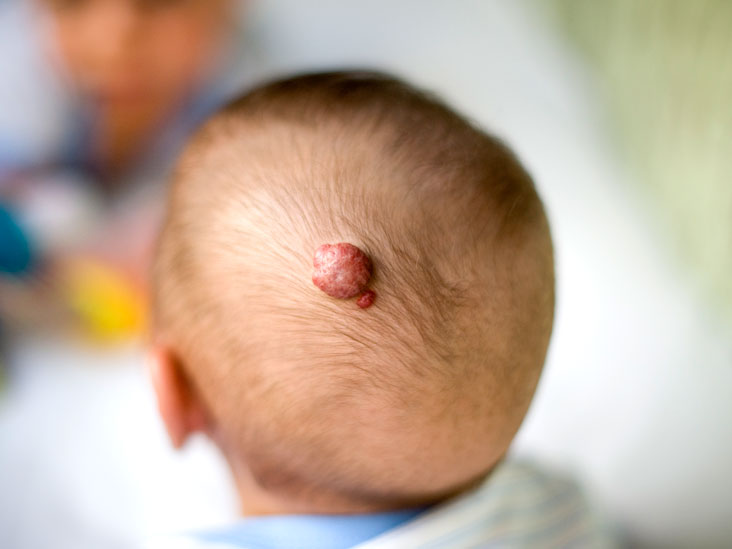
In a majority of cases, a hemangioma is harmless. However, they may be painful and can affect other organs in your body. Therefore, your doctor will want to rule out other diseases before recommending treatment for an individual. Internal hemangiomas can form in the brain, liver, and other parts of the body. In most cases, these tumors are small and do not produce symptoms, so they are often not noticed until you undergo a scan for a different condition.
Drugs That Inhibit Hemangioma Cell Growth
Bleomycin, a drug that inhibits the growth of hemangioma cells, is the most widely used medication for treating the condition. It is effective, safe, and easy to administer. It also has an acceptable fit index, indicating that it is a valid measure of QoL in children with hemangiomas. A hemangioma-QoL questionnaire is an excellent tool for assessing the quality of life of affected patients.
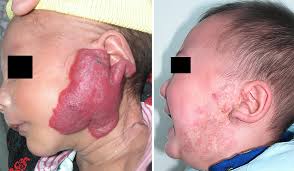
Children with hemangiomas will be at risk for stroke as the blood vessels in their bodies narrow. A lack of blood flow to the brain is very dangerous for the affected child or adult. They may also develop seizures or lose the feeling in one side of their body. Ultimately, these tumors are fatal if left untreated. When it is discovered, treatment should be sought immediately. If hemangiomas are left untreated, they will eventually spread throughout the body and may become painful.
Reference: