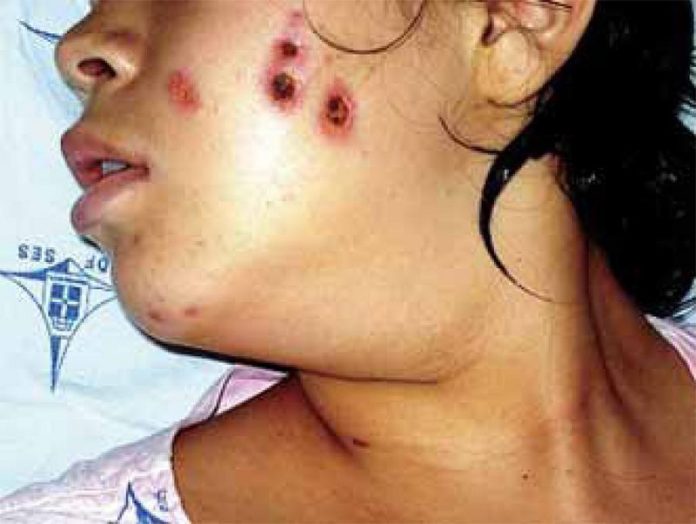
Dhealthwellness.com – The condition of Pyoderma gangrenosum begins as an erythematous papule, pustule, or nodule. These growths may coalesce into ulcers or ulcerative lesions with a raised, violaceous border. Initially, patients may experience pain, but the condition can also be a sign of hematologic disorders. Treatment depends on the severity of the lesions and can include topical corticosteroids, systemic steroids, or immunotherapy.
Common Symptoms of Pyoderma Gangrenosum
Symptoms of Pyoderma gangrenosum usually begin as a small, red bump, blister, or ulcer. Often, the sores have a raised border and ooze fluid. This type of ulcer can grow large and cause pain and an overall feeling of illness. People with pyoderma gangrenosum are typically ill, feverish, and may have a general sense of ailment.
This rare inflammatory neutrophilic dermatosis is characterized by red, painful swelling that may be accompanied by a skin injury. A skin biopsy will be required to confirm the diagnosis. However, immunosuppressive agents are often necessary in the management of PG. The disease is most easily treated with a medication called calcipotretin. Symptoms of Pyoderma gangrenosum can be treated with a course of immunosuppressants.
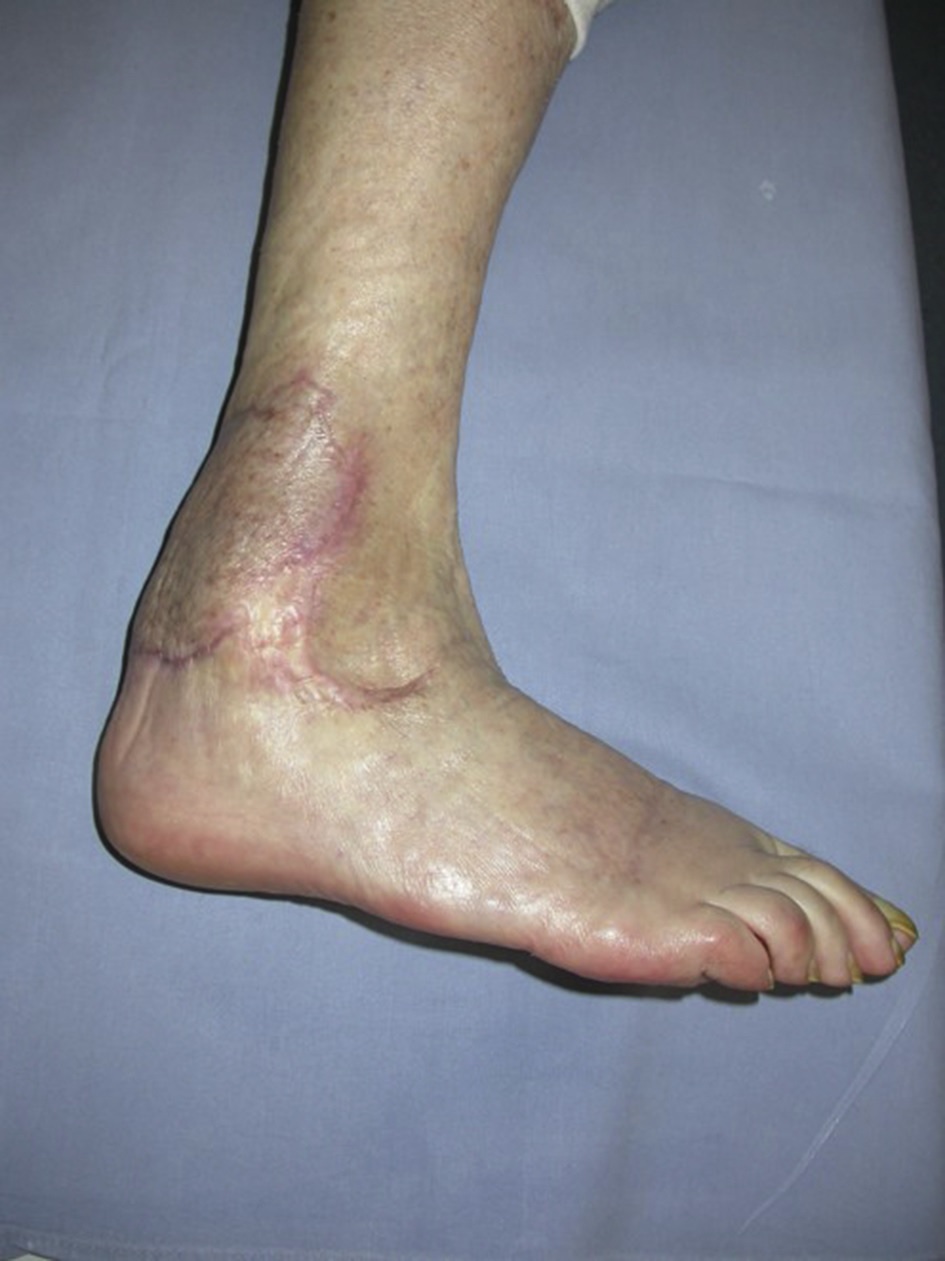
The diagnosis of Pyoderma gangrenosum can be difficult, but it is worth looking into. The condition can range from mild to severe and can leave unpleasant scars. If untreated, the condition can turn into a more serious condition. Primary care doctors should refer suspected patients to a dermatologist for a proper diagnosis. If a doctor suspects that a patient has PG, they should refer them to a dermatologist.
Pyoderma Gangrenosum Starts as a Red Bump
Unlike most other skin conditions, pyoderma gangrenosum usually starts as a red bump. It is more likely to occur on the lower legs, although it can affect the lungs, heart, or muscles of a patient. In severe cases, the condition can spread to the lungs, causing bleeding. The affected person may develop a fever or a general feeling of ill health.
Early treatment is important because the condition can spread very rapidly and leave painful scars. It is important to seek medical advice as soon as possible if you suspect it. There are several ways to treat pyoderma gangrenosum. Some people may have minor skin damage, but the condition can be related to another disease. Most cases have no obvious reason for the disease. While it is common to appear as a painful bump, it can also be associated with other symptoms.
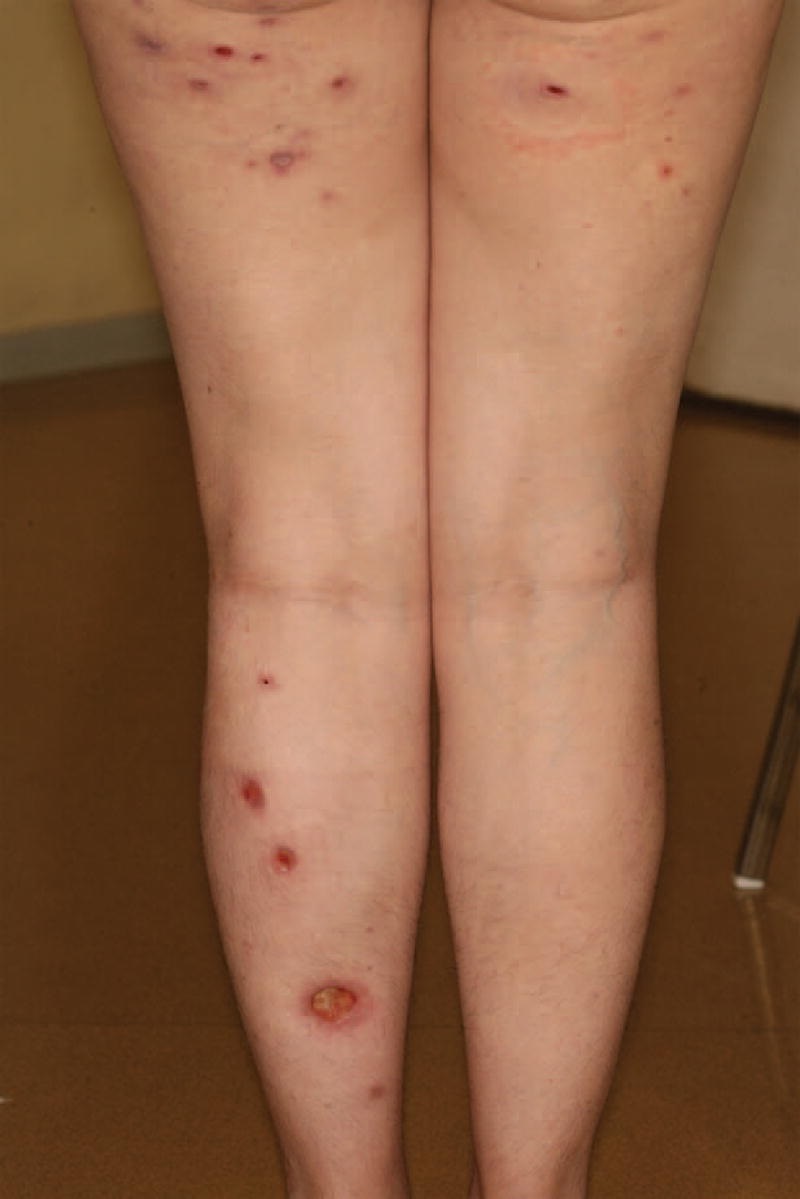
A pyoderma gangrenosum papule starts as a red bump but can also appear as a blister. In most cases, the sores have an elevated border. In some cases, it can turn into a large ulcer. In a more severe case, a pyoderma gangrenous ulcer can spread and become a full-blown ulcer. If left untreated, it can be fatal.
Diagnosing Pyoderma Gangrenosum
A physician can diagnose Pyoderma gangrenosum with the help of a skin biopsy. If it is associated with an infection, it is essential to seek medical care immediately. The condition can progress quickly and scarring is common. It can be difficult to treat, but early treatment reduces the risks of amputation and other complications. In some cases, it is best to consult a doctor for an accurate diagnosis.
Although the exact cause of Pyoderma gangrenosum is unknown, it is often accompanied by other diseases. Approximately half of people with PG also have another autoimmune disorder. In some cases, pyoderma gangrenosum is an autoimmune disorder, meaning the body fights itself. In other cases, the disease is a symptom of an underlying systemic disease. If the condition is severe, it can develop after an injury.
Symptoms of PG include deep, purulent ulcerations. In some cases, patients will require amputation of a lower limb, because the condition has no response to medication. Other symptoms may be similar to those of PG. The most common symptoms of the condition are pain, itchiness, and tenderness. In rare cases, the disease may affect the eyes or the lungs. Some of the symptoms of the condition an be fatal.
Reference: